Master's student enlisted as a contact tracer in the fight against COVID
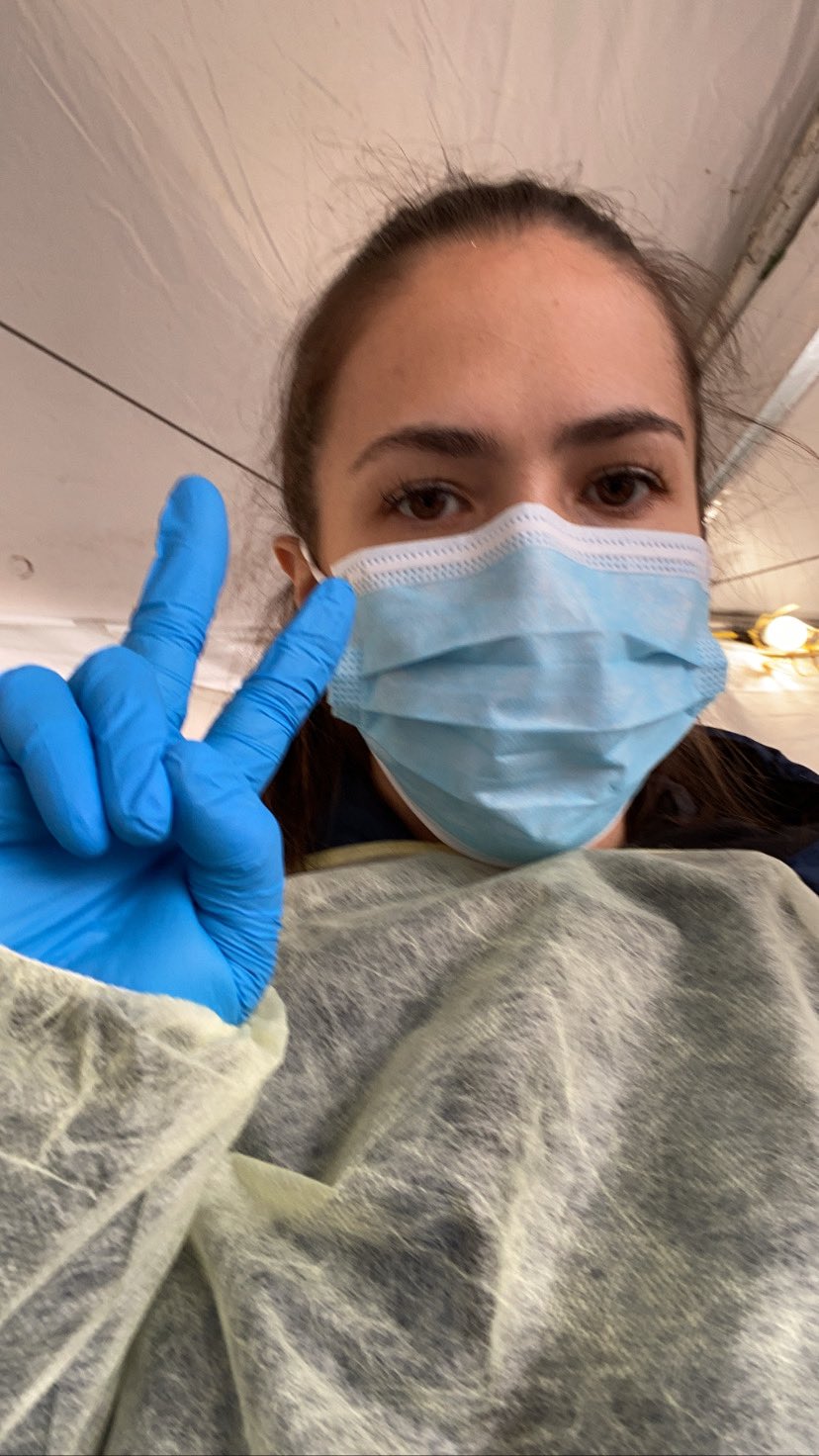
site in Dearborn
Corrinne Sanger, a master's student in medical anthropology, was working as an ethnographer and interviewer for a CDC-funded project called the National HIV Behavioral Surveillance study when the novel coronavirus (COVID-19) arrived in Michigan.
No longer able to conduct in-person interviews, the bulk of her work, Sanger was pulled from the research project and reassigned as a contact tracer for the CDC.
"Contact tracing was a smooth transition from the lengthy interviews I was used to doing with people at-risk or currently living with HIV," she said, "and I was already trained in security and confidentiality protocols for the state and federal governments."
In March, she took part in providing testing for first responders and health care workers exhibiting COVID-19 symptoms at a drive-through site in Dearborn, a collaborative effort between Wayne State University Physicians Group, Wayne State University Health Sciences and ACCESS.
"It was a lot of work and really hard to see so many sick people pull up in one day when we still had no idea how bad it would get," Sanger said.
She was only able to do it once before contact tracing took over her schedule. Sanger quickly began averaging 50-hour work weeks making phone calls to those who had tested positive for COVID-19 on top of a full class load, her work as an instructional assistant for Andrea Sankar's, Ph.D., anthropological methods class, and a competitive weightlifting hobby she refuses to give up.
These days, she has a little more breathing room--winter classes are over and more contact tracers have been added to the local effort. She now works as a contact tracer between 30 to 40 hours a week.
Every few days, Sanger receives a list of case report numbers of people who have tested positive for the virus.
"(COVID-19) is obviously a state-mandated reportable illness," Sanger said. "That means, along with HIV, measles, chickenpox, TB, and other infectious diseases, all testing information for any positive individuals must be reported to the state and local health department for further investigation."
She logs onto the secure state disease surveillance site and assigns the case numbers to herself. Then, she starts making phone calls around 9 a.m. She asks each contact to verify their date of birth to make sure she's talking to the right person, then goes through a standardized list of questions: the date the onset of symptoms occurred; symptoms experienced; any hospitalizations; job information, including the last day they were at work; any recent travel; pre-existing health conditions; and finally, information on close contacts.
This is only the first step in contact tracing. Another team will call those who have come in contact with these "lab-confirmed positives" to advise them to quarantine, offer testing, resources and symptom-monitoring, she said.
If Sanger interviews a health care worker, first responder, essential worker or anyone who experienced an onset of symptoms after going to a party, attending a church service, or visiting a nursing home, she reports that case straight to regional epidemiologists.
"These cases are not in trouble, but due to the nature of their work or contacts, it is important that they be prioritized to stop the spread of the virus in large or fragile settings," Sanger said. "For example, one of my cases was a traveling X-ray tech who, although provided with proper PPE, was visiting five to six nursing homes and assisted living centers a day for two days prior to becoming seriously ill himself."
These cases are the hardest and most nerve-wracking, Sanger said, because it takes a lot of time to make sure she sends the right emails asking all the right questions to the right people.
Sanger said most of the people she calls want to help but are apprehensive at first that she knows so much about them. When someone doesn't trust that she is who she says she is, Sanger confirms other personal information for them: the date they were tested, what street they live on. She's even allowed to send them a picture of her state ID badge.

Still, "I have been hung up on many times or accused of being a hacker."
Often, others clam up at workplace questions, thinking their answers could get them in trouble, she said. Sanger, then, reaffirms the information they provide is confidential and serves only to help them tackle the virus better.
"For example, because testing is still so limited, by giving me the information of contacts who have been symptomatic but not tested means they will be added to a list of probable positives, which gives the state a more accurate picture of those affected."
Her advice for those who have tested positive for COVID-19 and can expect a phone call from a contact tracer?
"Know that the more information you share the better. We don't share any confidential information outside of state and federal systems, and all of your answers will be de-identified for statistical purposes."
COVID-19 is a terrible thing to go through, she added, but cooperation helps health officials help so many others.
By Kristy Case, web editor/writer for the Wayne State University Graduate School.